Strategy and Solutions
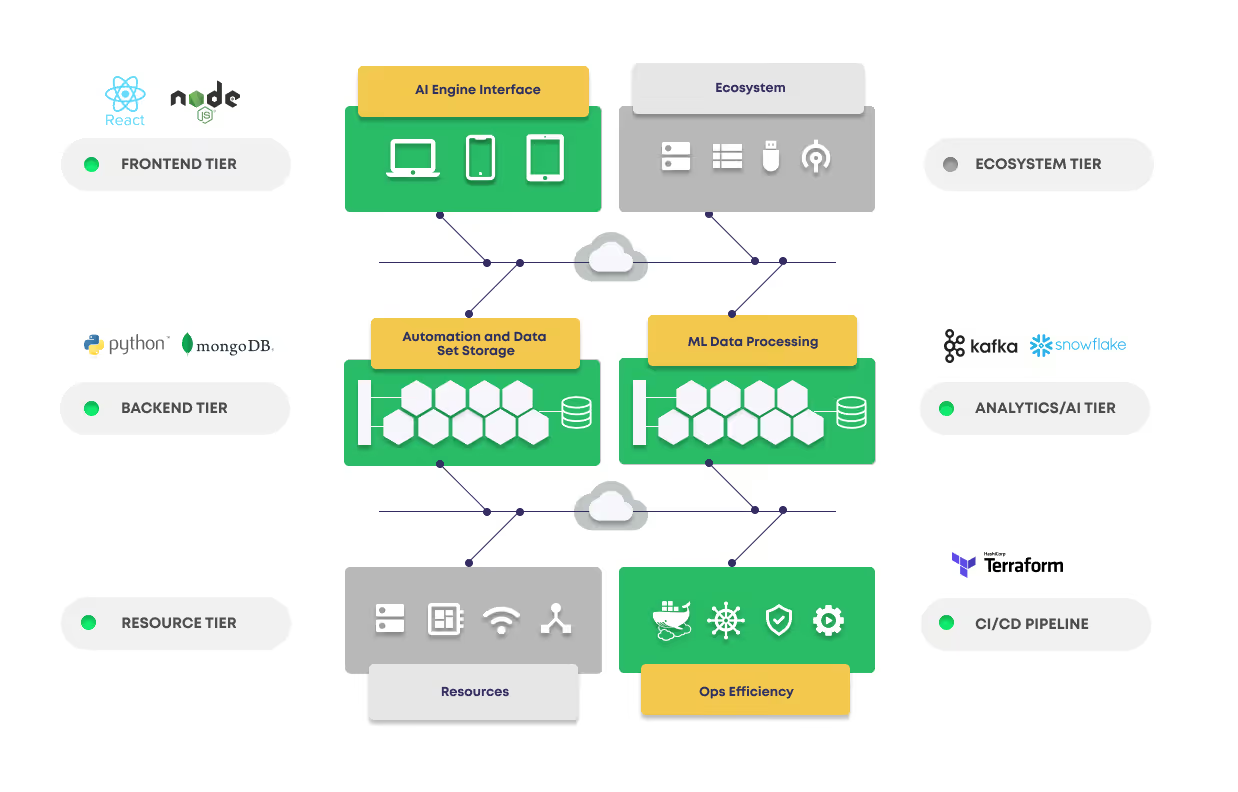
Zymr AI/ML services experts and healthcare IT services experts collaborated to develop an AI-native application with complete lifecycle management to AI-ML and MLOps to deliver significant value for our clients. The solution was deployed on Azure and built an AI solution with NLP, OCR, and related ML capabilities to extract competitive analysis of benefits and coverage. Our data science team was engaged with the client to understand the business objectives thoroughly and developed the ML model in consultation with the business stakeholders of our client. Our MLOps team architected a data ingestion pipeline, storing raw, feature-engineered, and golden data set in a SQL database. THE NER ML model was developed iteratively using BERT and spaCy. Several tools and technologies were used, such as Tessaract, AWS extract for OCR, neural nets, and fast text for data classification. Kafka played a crucial role in the continuous ingestion and distribution of health insurance documents from various sources. These documents are subsequently processed by the AI engine developed by our AI/ML services experts. Initially, the ingested bronze documents undergo document classification, followed by preprocessing stages involving OCR, by tesseract, and AWS extract. Text classification techniques such as BERT are applied, along with named entity recognition (NER) using Spacy or custom NER. Post-processing involves JSON conversion and storage. The user interface (UI) is developed using Node and React, while MongoDB stores the Bronze, Silver, and Gold data sets.










.svg)
.svg)
.svg)
.svg)
.svg)
.svg)
